Peptide therapy for healing has become one of the most-discussed tools in regenerative medicine, particularly for patients recovering from surgery, sports injuries, or persistent soft-tissue damage. If you’ve spent weeks waiting for a stubborn injury to resolve, or you’re staring down a recovery timeline that feels longer than it should, you’ve probably wondered whether there’s something beyond rest, ice, and physical therapy that could help your body heal faster.
The short answer is: maybe. Specific peptides have been studied for their effects on tissue repair, inflammation, and cellular regeneration, and at Good Chemistry in Cumming, GA, we use them as part of structured recovery protocols for the right candidates. This guide walks through what peptides are, which ones are used for healing, what the research actually says, and what to consider before starting therapy.
Table of Contents
What Peptides Are and How They Support Healing
Peptides are short chains of amino acids — essentially small proteins — that act as signaling molecules in the body. Your body produces thousands of them naturally, and each one tells specific cells to do specific things: repair tissue, reduce inflammation, regulate hormones, build collagen.
Therapeutic peptides used in healing protocols are designed to mimic or amplify these natural signals. When you give the body extra signaling capacity in the areas of inflammation control, blood vessel formation, and collagen synthesis, recovery can move faster and more completely than it would on its own.
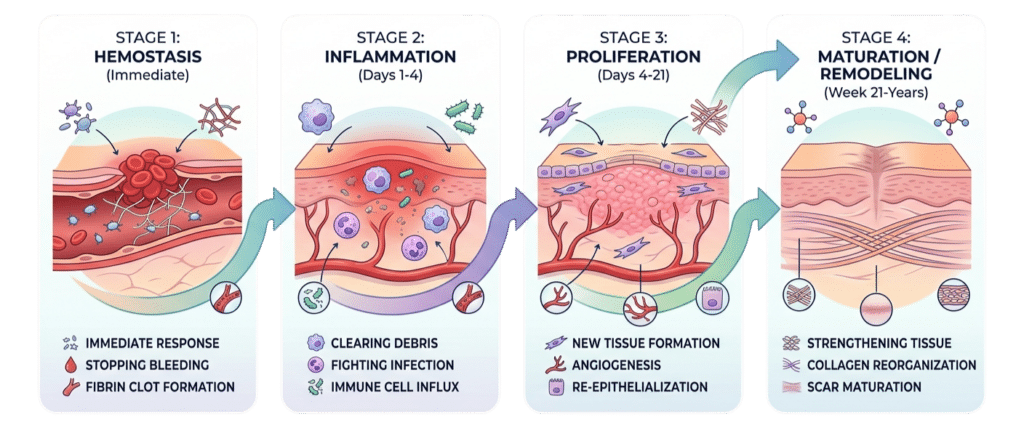
The peptides most commonly used for healing target three core processes: angiogenesis (the formation of new blood vessels to supply healing tissue), collagen production (rebuilding the structural matrix of skin, tendon, and ligament), and inflammation modulation (calming the prolonged inflammatory response that often delays recovery). Research on these mechanisms is growing, with peer-reviewed work in journals indexed on PubMed examining peptide effects on wound healing and musculoskeletal repair.
BPC-157 for Injury Recovery: The Most-Studied Healing Peptide
BPC-157 (Body Protection Compound-157) is the peptide most patients have heard about, and for good reason. It was originally isolated from a protective protein in human gastric juice, and research has examined its effects on tendon, ligament, muscle, and gut tissue repair.
What BPC-157 May Do
Studies — primarily in animal models, with some emerging human data — suggest BPC-157 for injury recovery may support healing through several mechanisms. It appears to promote angiogenesis at injury sites, accelerate tendon-to-bone healing, modulate inflammation without fully suppressing the healing cascade, and protect gastrointestinal tissue from damage caused by NSAIDs and other irritants.
The research is most established for soft-tissue injuries: tendinopathies, ligament strains, muscle tears, and post-surgical connective tissue repair. Patients dealing with stubborn injuries that haven’t resolved with conventional rehab are often the strongest candidates.
How BPC-157 Is Typically Administered
In clinical settings, BPC-157 is most often delivered via subcutaneous injection, sometimes near the site of injury when appropriate. Oral formulations exist but are generally considered less effective for systemic healing applications because of how the digestive tract processes peptides.
It’s worth noting that BPC-157 is not currently FDA-approved as a prescription medication. It’s available through FDA-registered facilities for legitimate medical use under physician supervision, which is how we work with it at Good Chemistry. The World Anti-Doping Agency has placed it on its prohibited list for competitive athletes, so anyone subject to drug testing should plan accordingly.
TB-500 (Thymosin Beta-4): The Other Major Healing Peptide
TB-500 is a synthetic version of a fragment of thymosin beta-4, a naturally occurring peptide involved in cell migration and tissue repair. Where BPC-157 is often described as targeting localized healing, TB-500 is more frequently used for systemic recovery and for injuries involving multiple tissue types.
What the Research Suggests
TB-500 has been studied for its role in promoting cell migration to injury sites, supporting blood vessel formation, and reducing inflammation in damaged tissue. Animal research has examined its effects on cardiac tissue, skin wounds, and muscle injuries.
In practice, peptide therapy programs often pair BPC-157 and TB-500 because they appear to work through complementary mechanisms. BPC-157 tends to act more locally and quickly, while TB-500 supports broader systemic recovery and may continue contributing to repair over a longer time horizon.
Candidates Who May Benefit
Patients who often respond well to TB-500 include those recovering from larger surgical procedures, those dealing with multi-site injuries, and athletes managing chronic overuse damage. As with BPC-157, it’s not FDA-approved and is used in clinical practice through compounding pharmacies under medical supervision.
Peptides for Post-Surgery Healing: What to Expect
Surgery — even minimally invasive procedures — places significant demand on your body’s repair systems. The inflammation response, tissue remodeling, and immune system activity that follow a surgical procedure can take weeks to fully resolve, and during that window, your body is essentially running a months-long construction project.
Peptides for post-surgery healing protocols are designed to support that construction project at the cellular level. The goal isn’t to override your body’s natural healing — it’s to give it more raw materials and clearer signals to work with.
Common Post-Surgical Applications
The procedures where peptide protocols are most commonly considered include orthopedic surgeries (rotator cuff repair, ACL reconstruction, joint replacements), cosmetic procedures with significant tissue manipulation, abdominal and hernia repairs, and spinal procedures. The shared thread is meaningful soft-tissue or connective-tissue repair work, which is exactly where peptides like BPC-157 and TB-500 have the most research behind them.
Timing Matters
When peptides are introduced relative to surgery affects what they can do. Some protocols start peptides several weeks before a planned procedure to optimize tissue health going in. Others begin in the early post-operative window to support the most active phase of repair. The right timing depends on the procedure, your baseline health, and your surgeon’s protocols — which is why coordination matters.
We always recommend that patients considering peptide therapy around a surgical procedure inform their surgeon. Most surgeons are unfamiliar with peptide protocols, but they need to know what’s in your system, especially if there are concerns about bleeding, immune response, or interaction with anesthesia.

Other Peptides Used in Healing Protocols
While BPC-157 and TB-500 get most of the attention, several other peptides may play supporting roles in recovery and injury repair.
GHK-Cu (Copper Peptide)
GHK-Cu is a copper-binding peptide studied for its effects on skin healing, collagen production, and antioxidant activity. It’s most commonly used topically for skin repair after procedures, but injectable forms are also used in some recovery protocols. Research published through institutions like the National Institutes of Health has examined its mechanisms in wound healing and tissue regeneration.
Thymosin Alpha-1
Thymosin alpha-1 is primarily an immune-modulating peptide rather than a direct tissue-repair peptide, but immune function is deeply tied to recovery. Patients with chronic infections, autoimmune complications, or compromised immune response may use it as part of a broader recovery strategy.
IGF-1 LR3 and CJC-1295/Ipamorelin
These peptides work through the growth hormone axis and may support recovery indirectly by improving sleep quality, lean tissue repair, and overall regenerative capacity. They’re more commonly used in longevity and performance protocols than acute injury recovery, but they can play a role for patients dealing with extended recovery timelines.
The right combination depends entirely on the individual — what you’re recovering from, your baseline health markers, your other medications, and your goals. There is no universal “healing stack.”
What Peptide Therapy for Healing Cannot Do
This part matters as much as the benefits. Peptide therapy is not a replacement for conventional medical care, surgery when surgery is indicated, or physical rehabilitation. It works best as one component of a larger recovery strategy that includes appropriate rest, progressive loading, nutrition, sleep, and clinical oversight.
Peptides also don’t work equally well for everyone. Patients with certain underlying conditions, active malignancies, or specific medication regimens may not be candidates. Outcomes vary considerably based on the injury type, how long the condition has persisted, and individual biology.
It’s also worth saying directly: the research base for healing peptides is growing but still incomplete. Much of the foundational data comes from animal studies, and large-scale human clinical trials are still limited for many of these compounds. We use them in clinical practice based on the strength of available evidence, mechanistic plausibility, and a careful safety profile — but anyone telling you peptides are a guaranteed cure is overselling.
What a Peptide Therapy Program Looks Like at Good Chemistry
At Good Chemistry, peptide therapy starts with a comprehensive consultation and lab work. We’re not interested in handing peptides to anyone who walks in asking for them — the protocol needs to fit the person, the injury or recovery situation, and the broader health picture.
The Initial Workup
Your initial visit includes a detailed history of the injury or surgical situation, a review of medications and supplements, baseline lab work, and a discussion of goals and expectations. For post-operative patients, we coordinate timing carefully and typically want to see surgical notes and any imaging.
The Protocol
Once a protocol is determined, peptides are typically self-administered via subcutaneous injection on a schedule that matches the healing window. Most protocols run 4 to 12 weeks depending on the situation. We provide all training, supplies, and ongoing support, and we check in throughout the protocol to assess response and adjust as needed.
Integration With the Rest of Your Care
Peptide therapy works best alongside the rest of what your body needs to heal: adequate protein intake, sleep, movement appropriate to the recovery stage, and any prescribed physical therapy. We coordinate with your surgeon, physical therapist, or primary care provider when relevant.

How much does peptide therapy cost in Cumming, GA?
Peptide therapy at Good Chemistry is priced based on the specific peptide protocol, dosing, and program length. Most healing-focused protocols run 4 to 12 weeks and pricing reflects both the medication and the clinical oversight involved. Many patients find that bundling peptide therapy with our hormone therapy membership makes ongoing protocols more accessible. We provide exact pricing during your consultation once we’ve determined the right protocol.
Is BPC-157 safe?
BPC-157 has a generally favorable safety profile in the available research, with most studies reporting minimal adverse effects at therapeutic doses. That said, it’s not FDA-approved, long-term human data is still limited, and individual response varies. Patients with active cancer, certain cardiovascular conditions, or specific medication regimens may not be candidates. We review your full history and current medications during your peptide therapy consultation before recommending any protocol.
How long does it take to see results from peptide therapy for healing?
Most patients begin noticing changes within 2 to 4 weeks, though meaningful tissue repair takes longer. Acute injuries and post-surgical patients often report faster perceived recovery, while chronic injuries may need 8 to 12 weeks before significant change is evident. Results depend heavily on the injury type, how long it’s persisted, and how well the rest of your recovery is supported. We track progress at scheduled check-ins throughout your recovery protocol and adjust as needed.
BPC-157 vs TB-500: which one do I need?
It depends on the injury. BPC-157 tends to work more locally and quickly — strong for tendon, ligament, and gut-related injuries. TB-500 supports broader systemic repair and is often used for multi-site injuries, larger surgical recoveries, or chronic overuse damage. Many of our protocols combine both because their mechanisms are complementary. The right answer comes from your specific situation, which we’d evaluate during your initial consultation.
Can I use peptide therapy after cosmetic surgery?
Yes, peptide therapy is commonly used to support recovery after cosmetic procedures involving significant tissue manipulation. Timing and protocol selection should be coordinated with your surgeon to avoid any conflict with their post-operative protocols. We often recommend patients plan their peptide therapy around their surgical timeline so the medication is supporting the most active phase of repair. Reach out through our contact page to discuss your specific procedure timing.
Are peptides legal?
The peptides we use clinically — including BPC-157 and TB-500 — are sourced from a US-based, FDA-registered laboratory and dispensed under physician supervision for legitimate medical use. They are not FDA-approved as prescription medications, which is an important distinction. They’re also on the World Anti-Doping Agency prohibited list, so competitive athletes subject to drug testing should not use them. Our medical director oversees all peptide protocols at the practice.
Is Peptide Therapy for Healing Right for You?
Peptide therapy isn’t the right tool for every recovery situation, but for the right candidate — someone with a soft-tissue injury that’s been stubborn, a planned surgery where optimized recovery matters, or a post-operative situation where the standard timeline feels too long — it can be a meaningful addition to a recovery plan.
The most important step is honest evaluation. That means lab work, a thorough history, a realistic conversation about what peptides can and can’t do, and coordination with the rest of your medical care. We do that work upfront because peptides only deliver on their potential when they’re matched to the right person and the right situation.
If you’re recovering from surgery, dealing with a persistent injury, or planning a procedure and want to explore whether peptide therapy could support your recovery, we’d be glad to talk through it with you. Good Chemistry is located at Cumming City Center in Cumming, GA, and we offer Saturday appointments to make consultations easier to fit into your schedule.
Individual results vary. Peptide therapy is not FDA-approved and is used clinically under physician supervision. Schedule a consultation to determine if peptide therapy is right for you.
Book your peptide therapy consultation at Good Chemistry →
The Science of Feeling Good | Med Spa in Cumming, GA
- What the Research Says About Retatrutide in Cumming GA: A Look at the Most Promising GLP-1 Yet
- The Peptide Therapy Clinic in Cumming, GA Changing the Way People Age and Heal
- Peptide Therapy for Healing: 7 Science-Backed Benefits
- Transformative Tesamorelin in Cumming, GA: The Eager Solution for Stubborn Belly Fat
- You’re Not Just ‘Getting Older’ — You Might Just Need Hormone Optimization in Cumming, GA
